Delayed implantation and immediate loading in a teenager in the esthetic zone
Doc. MUDr. Martin Starosta, Ph.D.
- Dr. Martin Starosta completed his dental education at Palacky University in Olomouc, Czech Republic, followed by a residency at the Clinic of Stomatology, University Hospital Olomouc.
- In 1999, he was appointed as a forensic expert in forensic dentistry.
- Dr. Starosta assumed leadership of the Department of Dentistry at the University of Ostrava‘ s Faculty of Medicine in 2023, while continuing to operate his private practice in Olomouc.
- He is a member of the Committee of the Czech Periodontology Society and belongs to international organizations such as the European Federation of Periodontology (EFP) and the International Team of Implantology (ITI). Dr. Starosta regularly contributes to his field through professional reports, scientific articles, and textbooks, and is a respected speaker at conferences both in the Czech Republic and internationally.
Anamnesis
An 18-year-old female patient sought treatment for a persistent fistula on tooth 21. The issue stemmed from a bicycle accident five years before, which had injured her upper lip and subluxated the affected tooth. Initially, the soft tissue was sutured, and the tooth repositioned, with follow-up care provided by her dentist. A year after the accident, the patient noticed discoloration of the tooth, prompting a series of endodontic treatments. Due to the tooth‘s increased mobility, it was stabilized using a composite splint connecting it to the adjacent teeth.
Clinical casebook
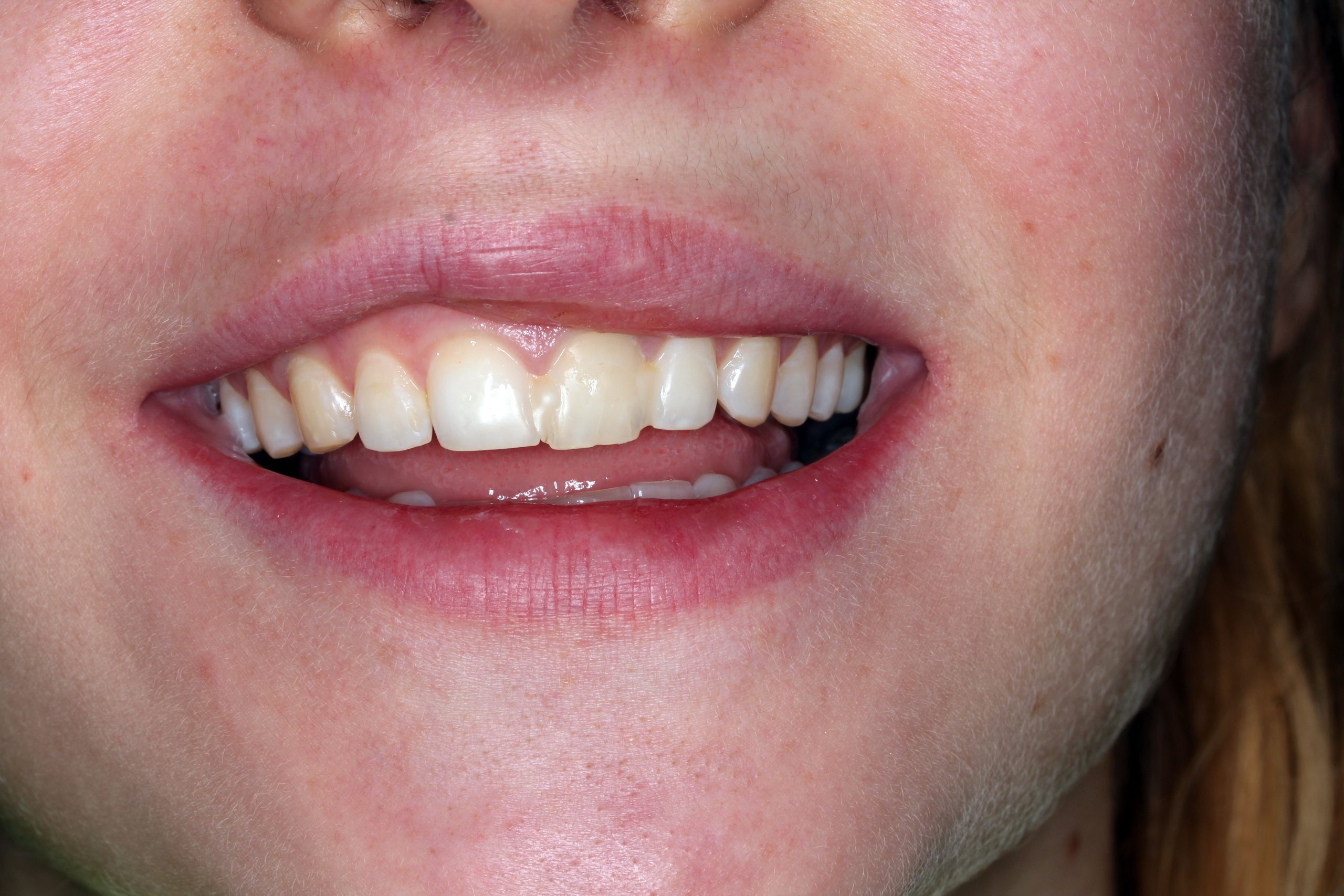
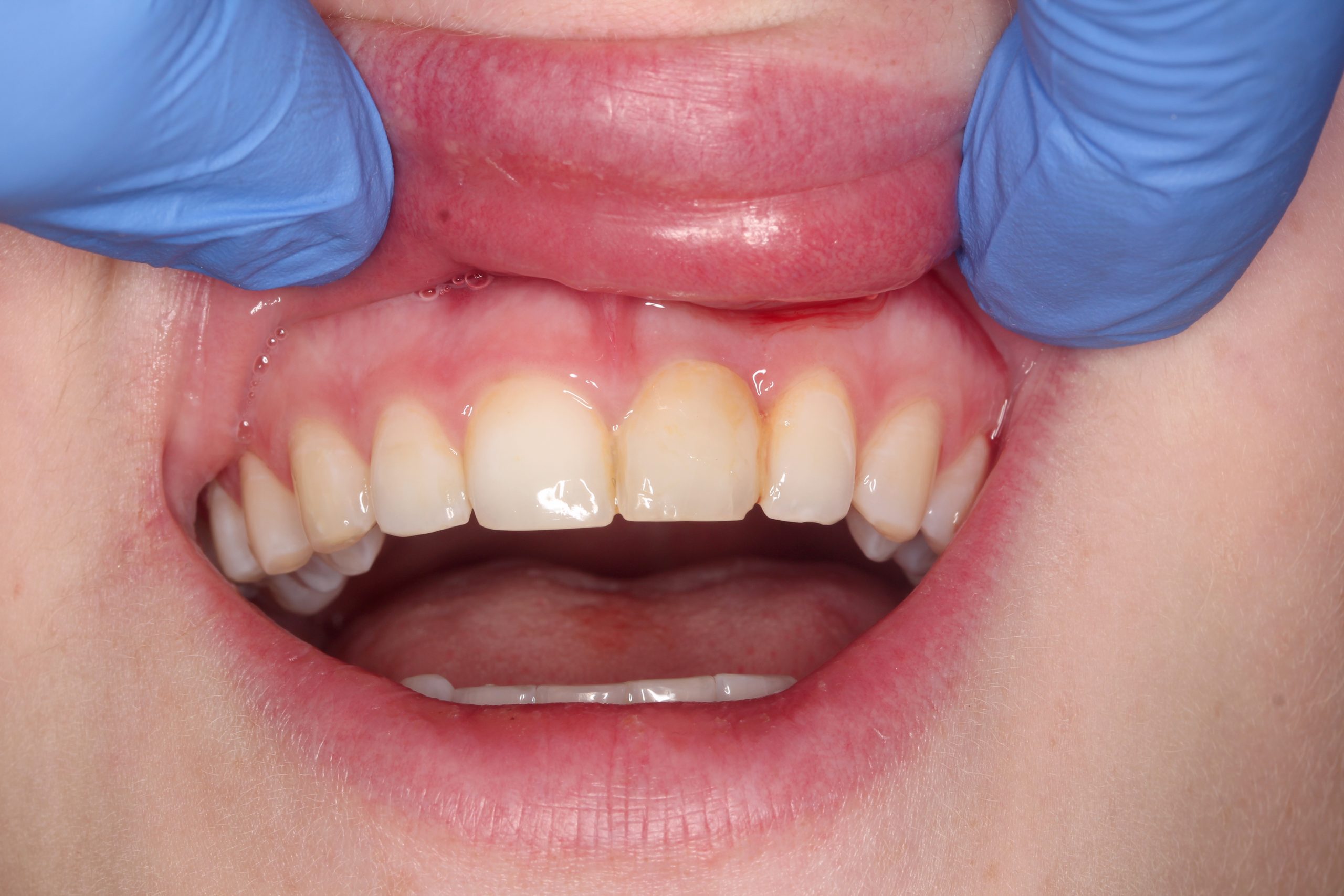
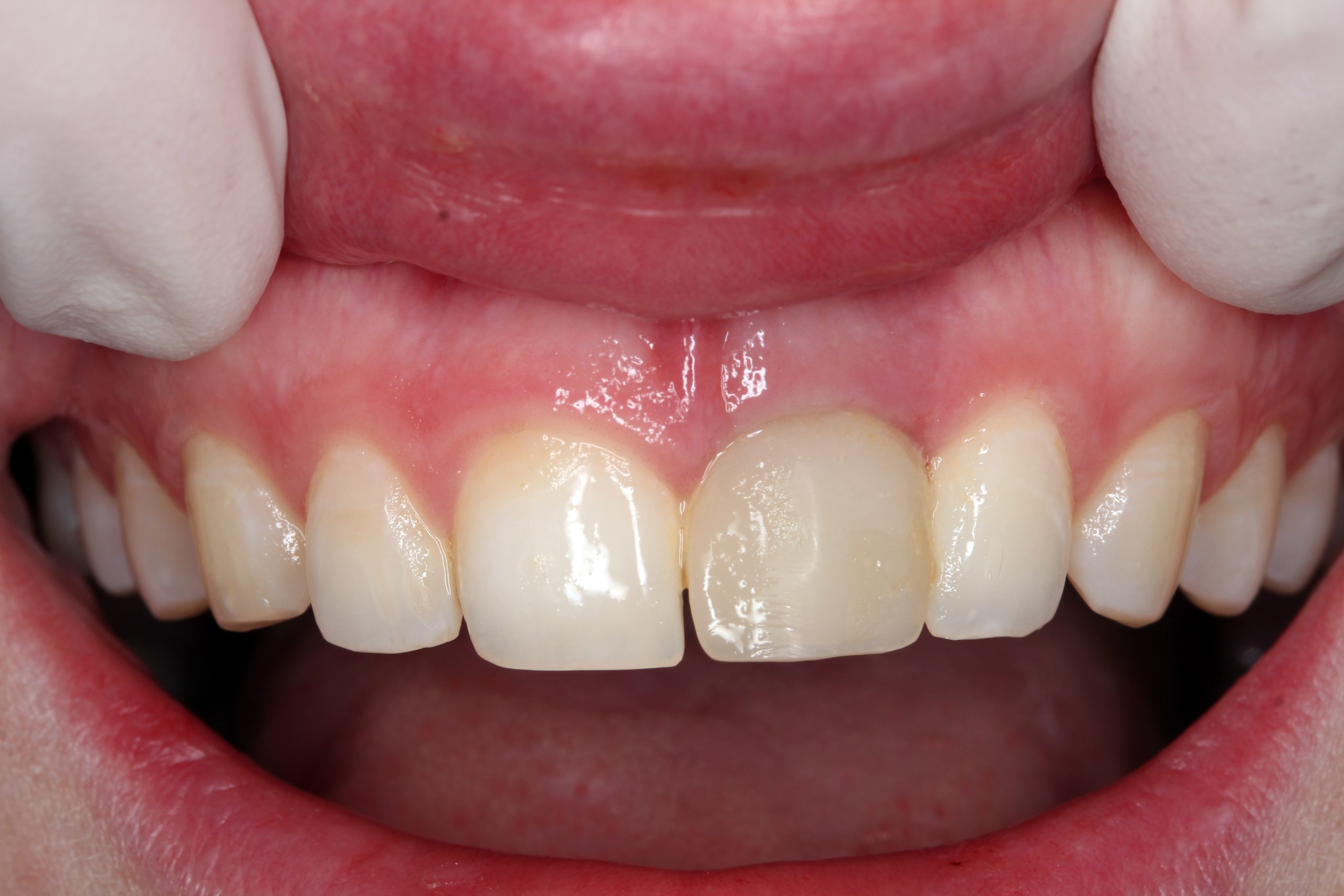
Initial situation: The irregularity of the smile line was caused by a deformation of the lip due to trauma.
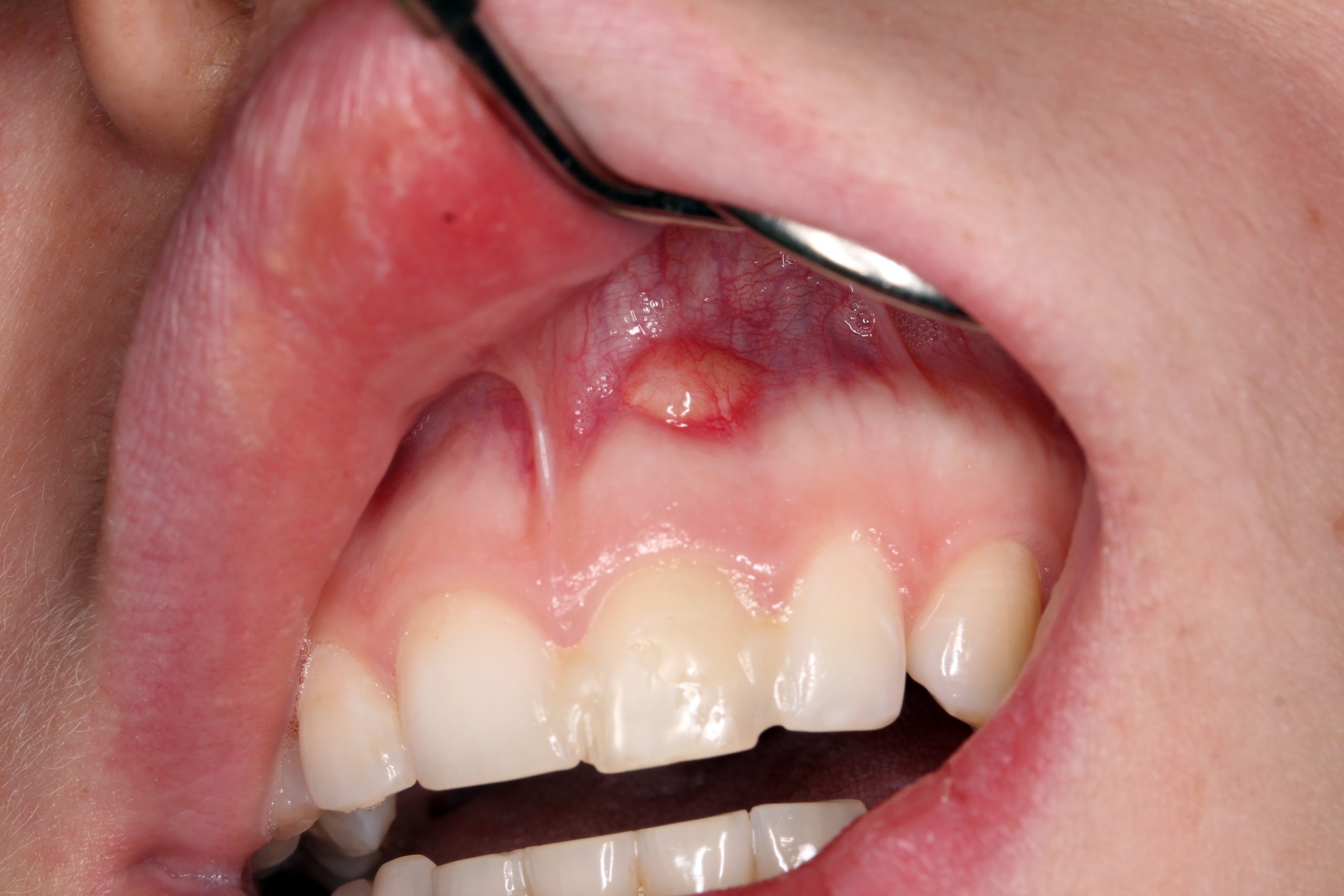
A chronic fistula in region 21. The blocked tooth 21 with a different discoloration. The intraoral radiograph 21 confirmed incomplete endodontic treatment and partial root resorption.
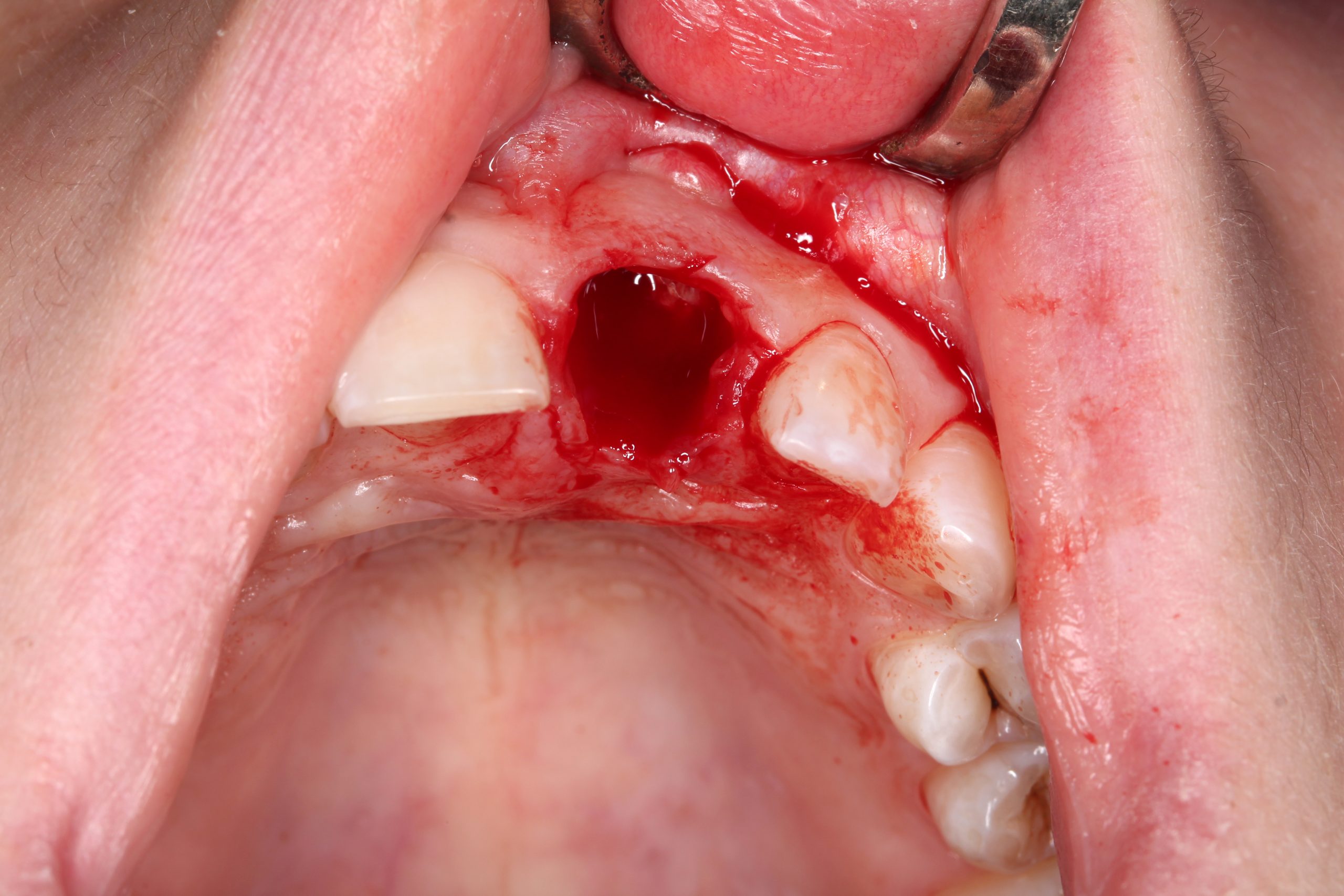
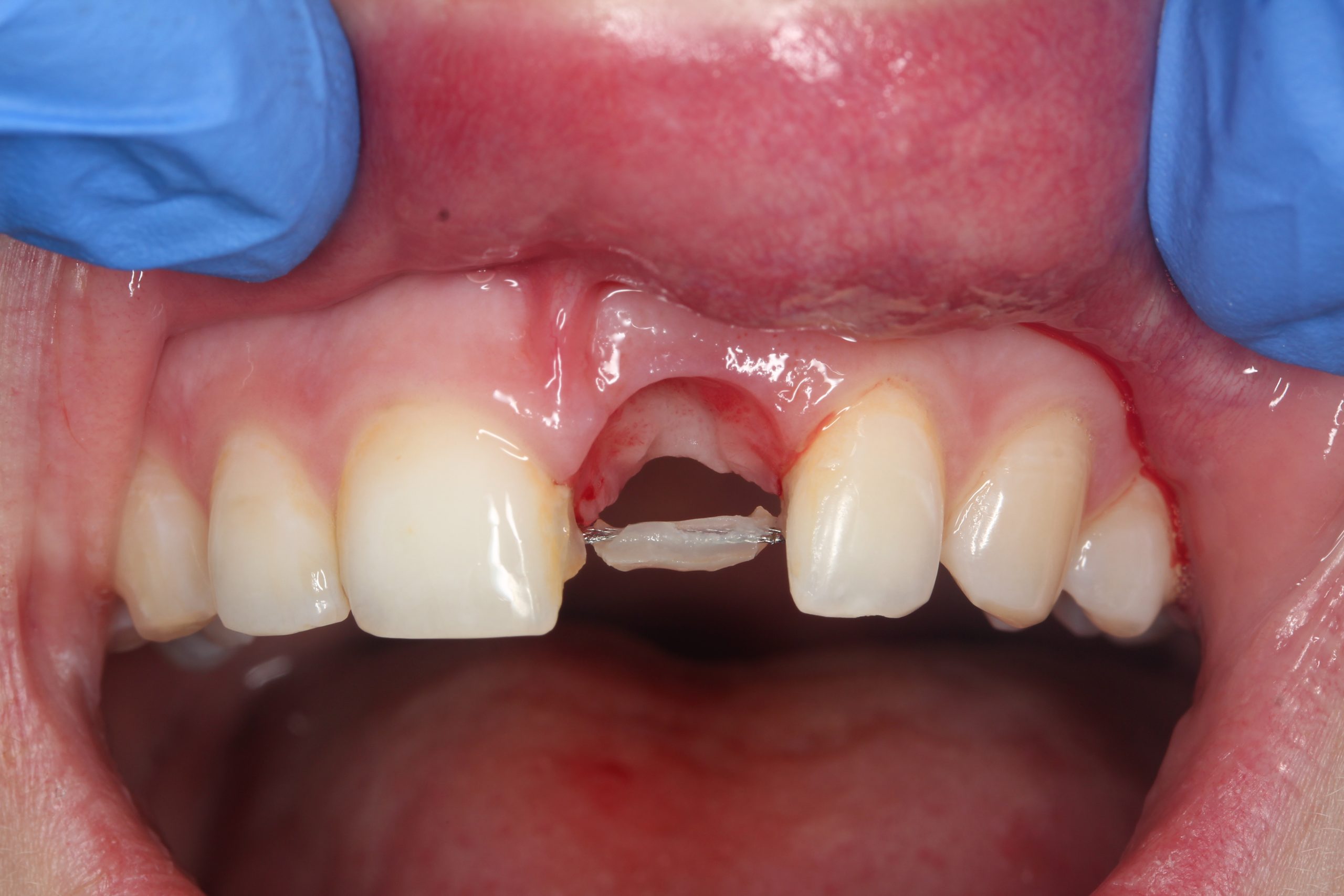
After extraction and excochleation, the extraction wound was revised. The vestibular wall of the socket was preserved except for the apical part. The tooth bed was only filled with an antibiotic-containing collagen cone.
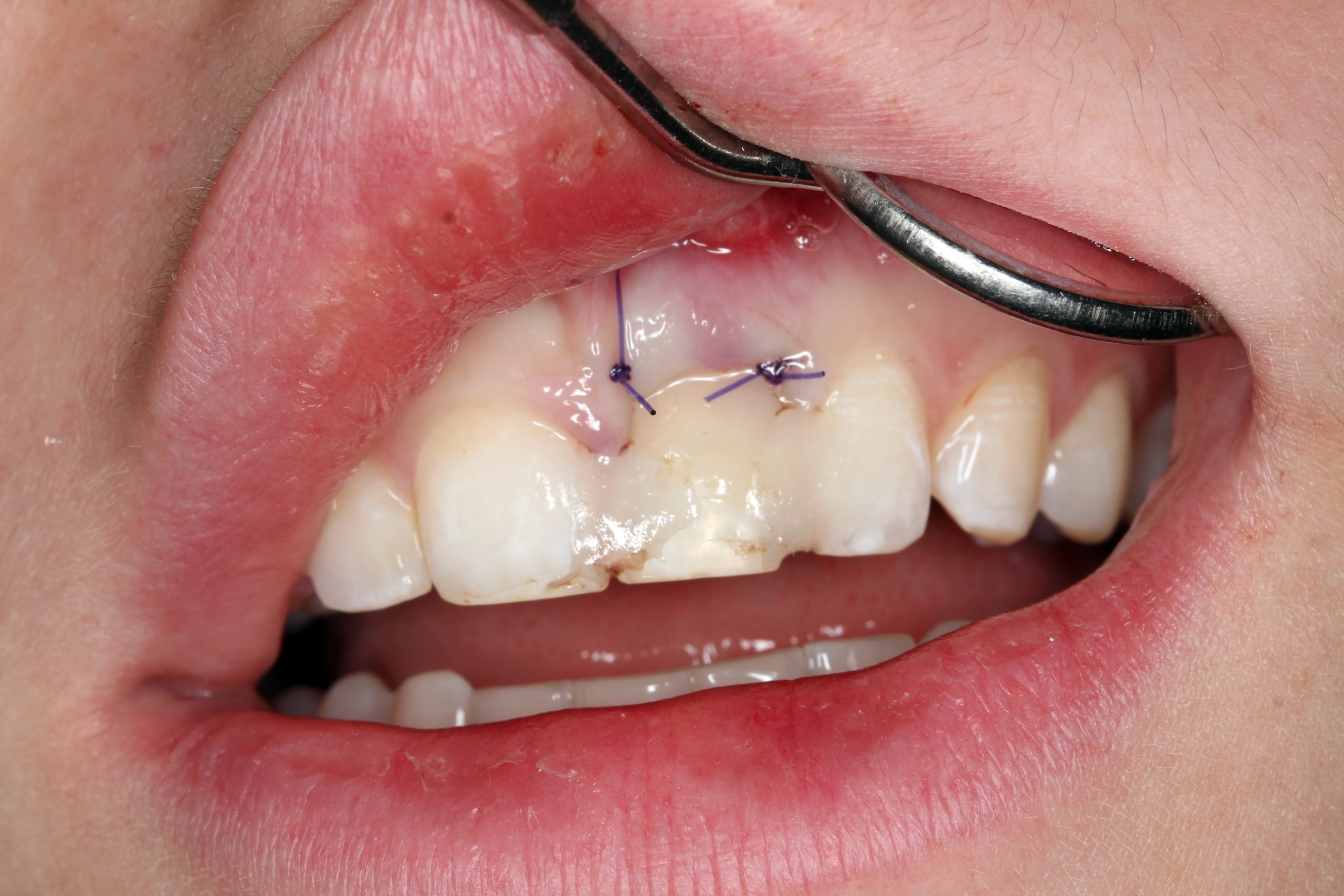
The extracted tooth was used as a temporary restoration. The root was cut approximately 2 mm below the CEJ so that this part was embedded in the soft tissue. The crown was cemented to the adjacent teeth with composite.
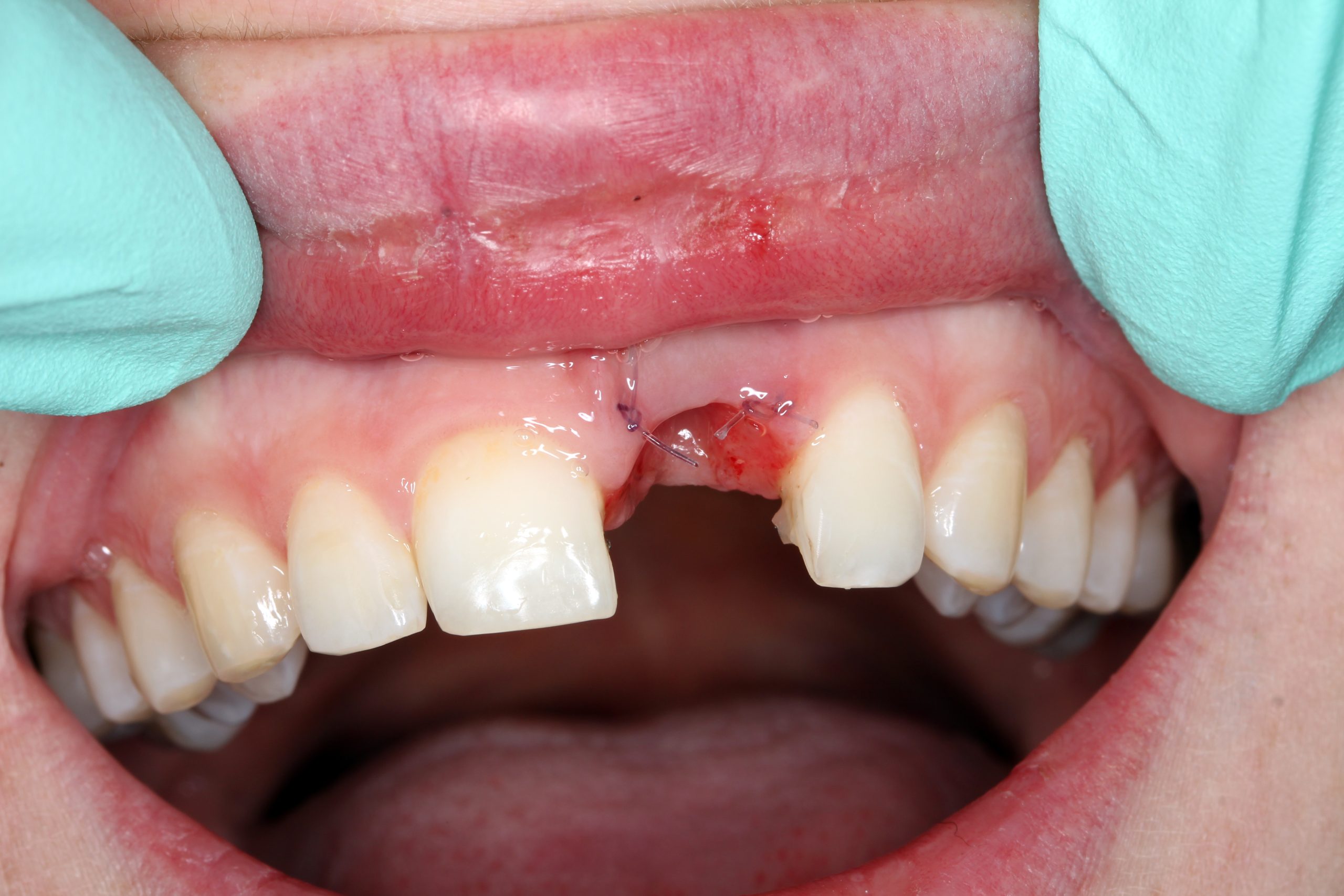
After 14 days, we checked the healing and fixed the tooth again with a multi-strand wire from the palatal side.
Situation after one month. Immediate loading of the implant was planned. The preliminary impression was used to fabricate a temporary crown.
After removal of the crown: a perfectly epithelialized extraction site and preserved interdental papillae. The wire splint with which the dental crown had been temporarily fixed was temporarily retained as a control element for inserting the implant.
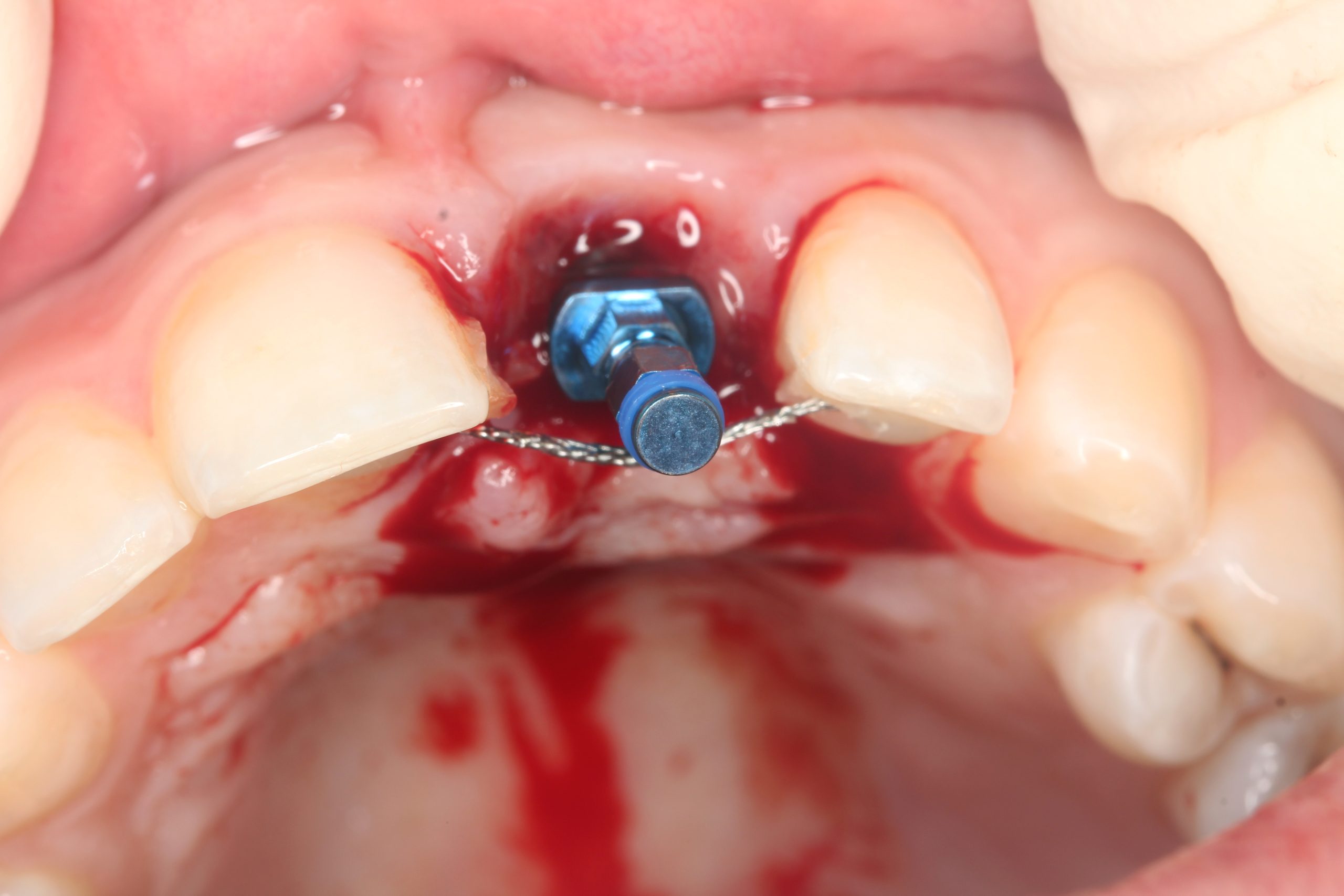
The mucoperiosteal flap was lifted palatally and partially mobilized vestibularly. A 14 mm long BioniQ implant from LASAK with Ø 4 mm was inserted and a temporary abutment was attached after removing the implant carrier.
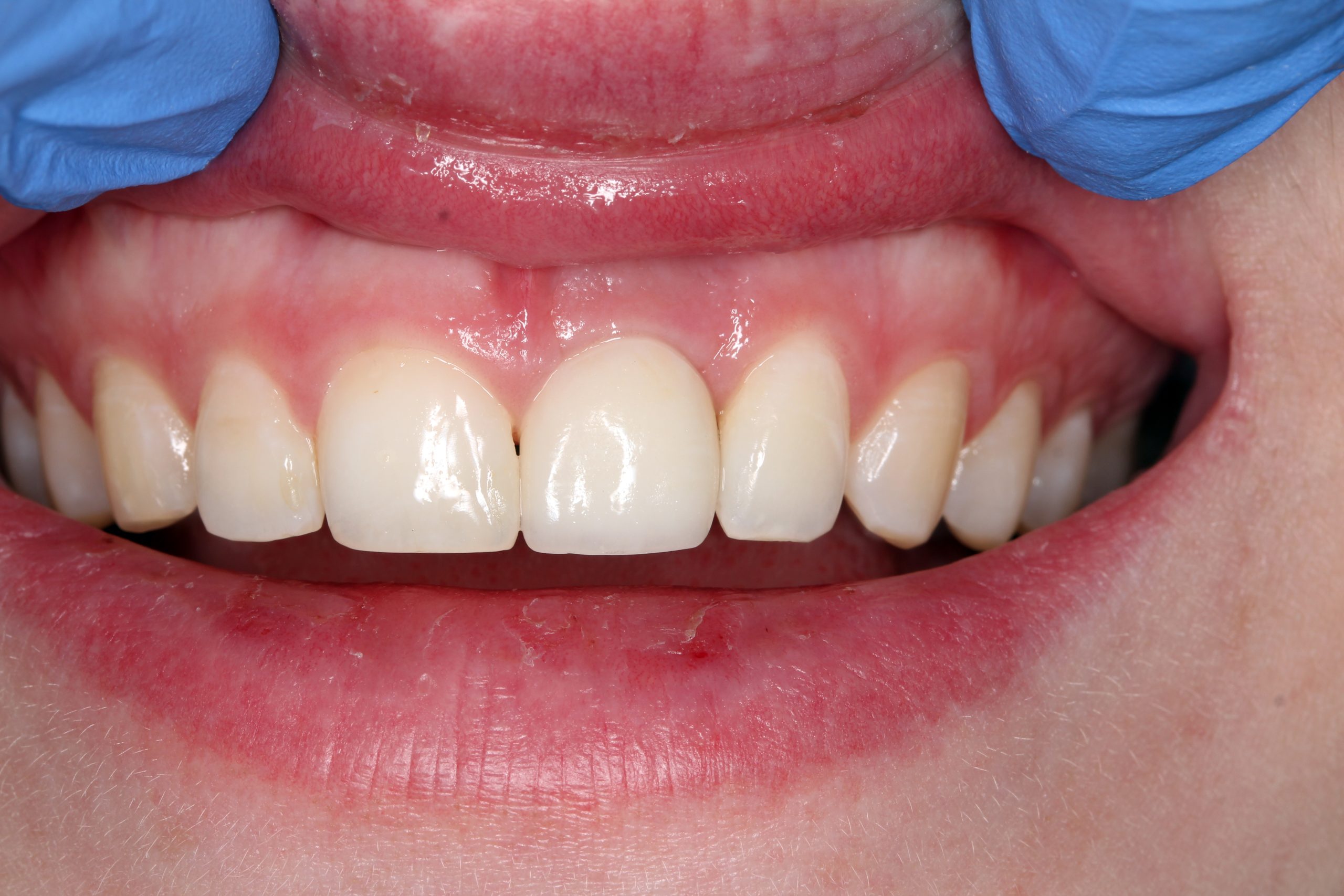
No problems occurred at the one-month follow-up. The temporary prosthesis was integrated into the surrounding tissue and the esthetics of the soft tissue were preserved.
Four months after implant placement and immediate loading, the temporary crown was removed. An all-ceramic crown was fabricated in the laboratory.
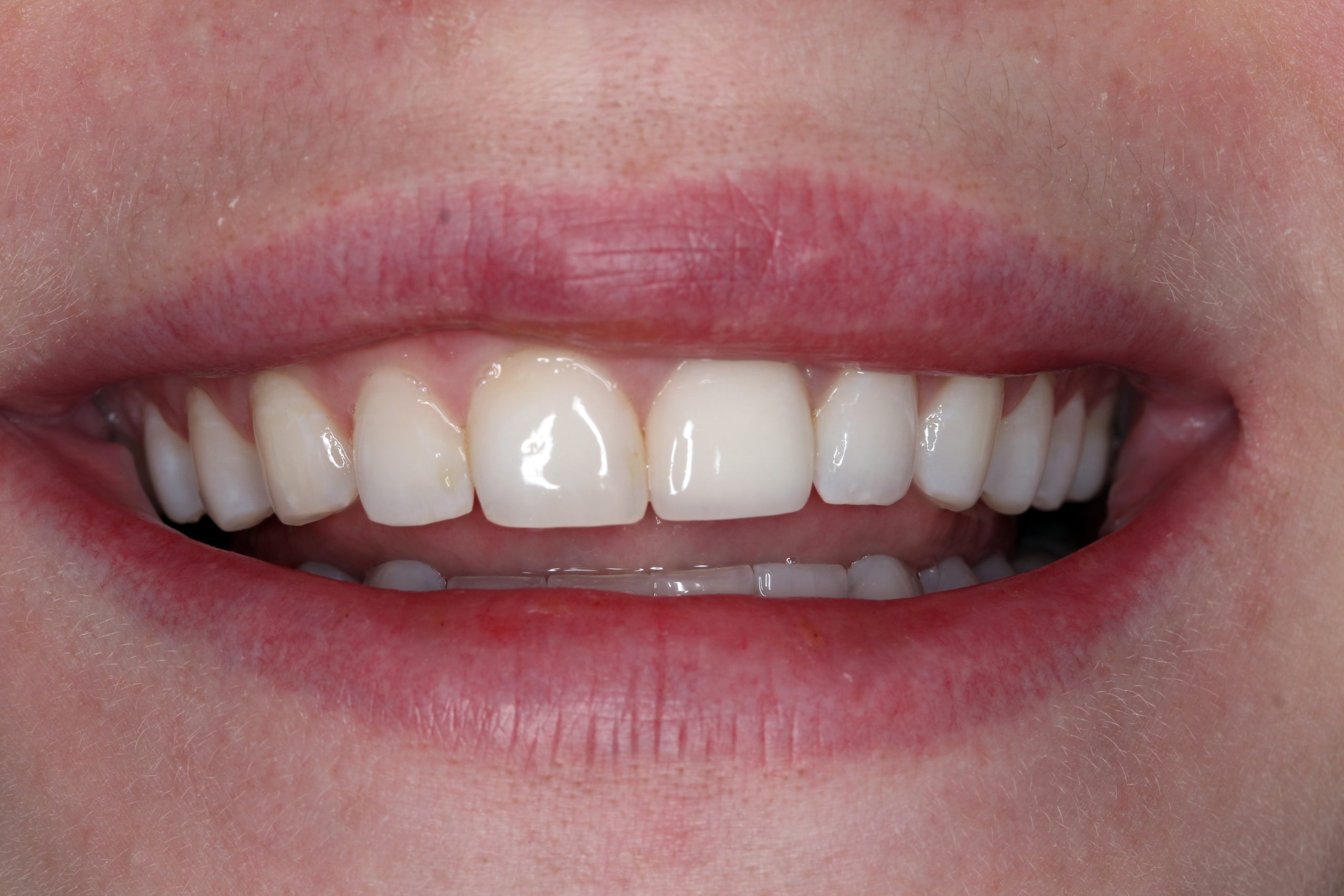
The patient‘s smile at the recall after three years. Minimally invasive surgical procedures and preservation of the surrounding tissue made it possible to achieve the best possible esthetic and functional result.
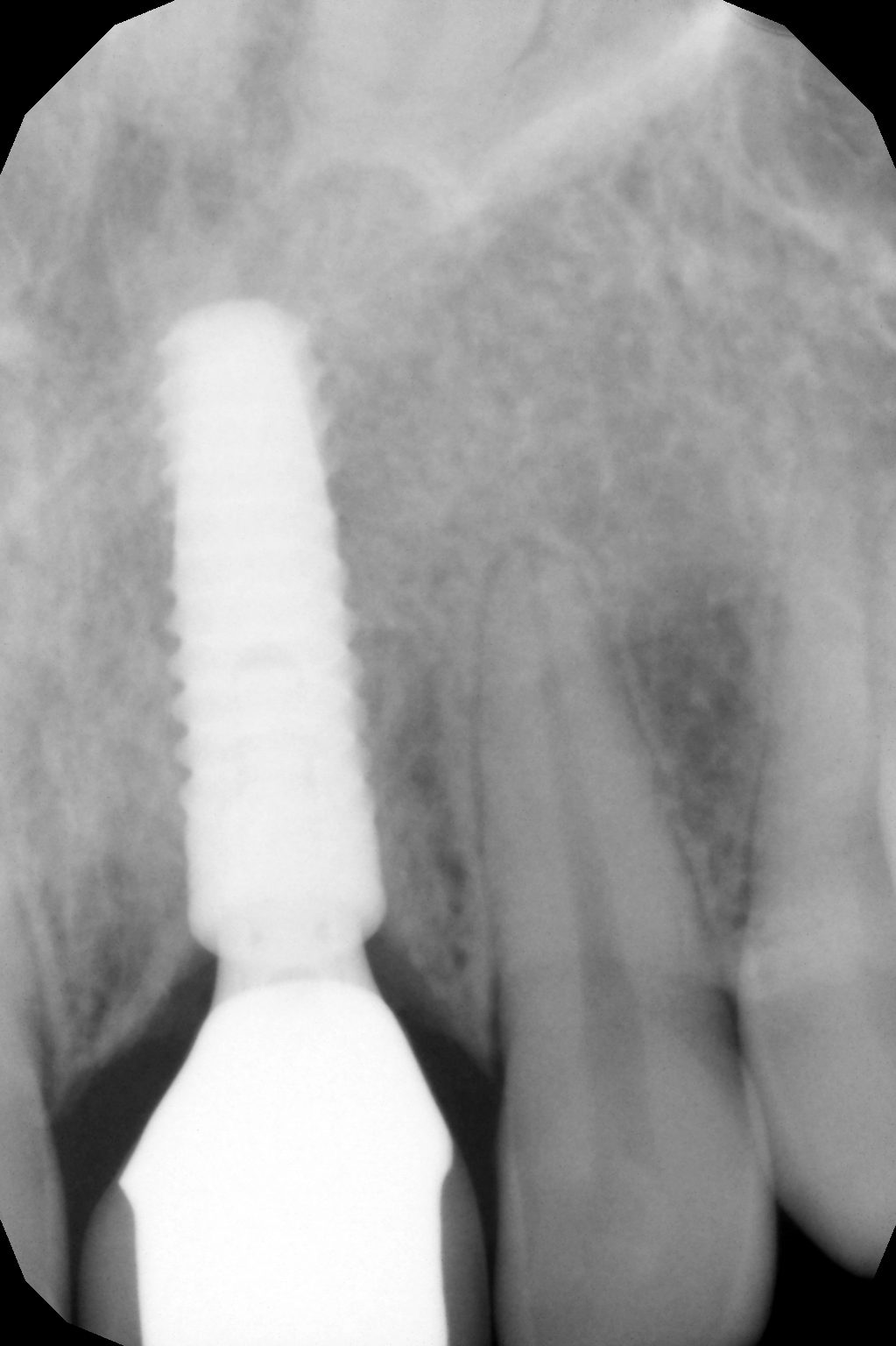
The X-ray after three years also shows a healed socket without resorptive changes.
Here you can download clinical casebook